I went in for routine bloodwork expecting… nothing. Instead, I got a number that stopped me in my tracks. My C-reactive protein (CRP) came back at 41. For context, normal is under 3.
CRP is a marker of inflammation, and when elevated, it can signal an increased risk of cardiovascular issues, including heart disease and stroke. I didn’t feel sick. I didn’t feel like anything was wrong. And that’s what made it unsettling.
We repeated the test. This time, it came back at 19. Better, but still significantly elevated. That’s when things shifted from “let’s watch it” to “let’s investigate further.”
The Next Step: A Cardiac Stress Test
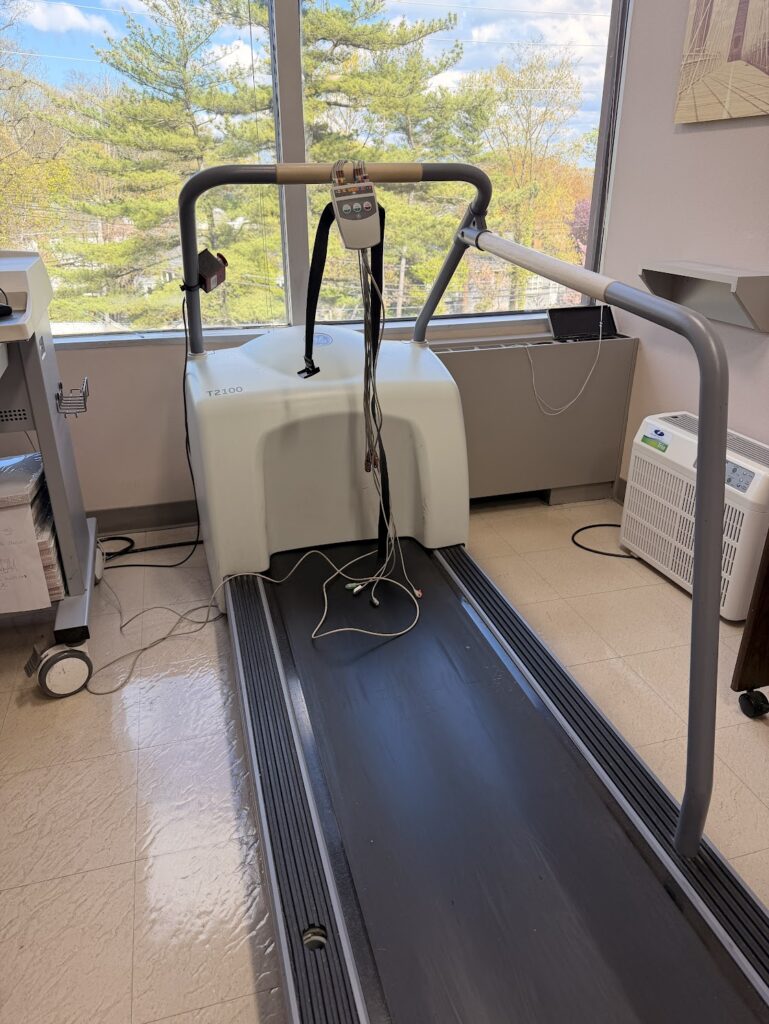
My doctor recommended a cardiac stress test. If you’ve never had one, here’s the simple version:
It’s a test that measures how your heart performs under physical stress, usually while walking on a treadmill.
Because here’s the thing:
Your heart can look completely fine at rest…
but show problems when it’s working harder.
What the Stress Test Actually Feels Like
This is what I wish someone had told me beforehand. You’re hooked up to monitors. They track your heart rate, rhythm, and blood pressure. You start walking slowly.
Then:
- The speed increases
- The incline increases
- Your heart rate climbs
The entire time, they’re watching how your heart responds.
I immediately had trouble breathing. ON THE FIRST ROUND. Every three minutes, they push you a bit further out of your comfort zone, but right off the bat, I was struggling. I guess that was my first clue?
My Results: “Indicators” That Needed a Closer Look
My results showed possible indicators of blockage. That word alone is enough to send your mind spiraling. But here’s something important I’ve learned:
A stress test doesn’t diagnose everything. It flags concerns. This is why my next step is a stress test with an echocardiogram.
Stress Test vs. Stress Echo: What’s the Difference?
A regular stress test:
- Tracks the electrical activity of your heart (EKG)
- Monitors heart rate and rhythm
A stress echocardiogram adds imaging:
- Uses ultrasound to actually see your heart
- Shows how blood flows through it
- Can reveal areas not getting enough oxygen
In simple terms:
- One listens to your heart
- The other watches it
And that added layer can detect issues a basic test might miss.
The Emotional Side No One Talks About
This part matters just as much as the medical side. Because when you hear:
- “inflammation”
- “blockage”
- “heart”
…it’s easy to go straight to worst-case scenarios. But here’s what I’m holding onto: This process is about information, not panic. Stress tests are designed to uncover hidden issues early, even in people who feel completely fine. And early detection? That’s power.
Signs You Shouldn’t Ignore
Even though many heart issues are silent, some symptoms can show up:
- Shortness of breath
- Chest discomfort (even mild)
- Unusual fatigue
- Heart palpitations
- Feeling off during exertion
But here’s the truth: You can have none of these… and still need to pay attention.
What to Expect at Your Appointment
If you’re heading into this yourself:
- Wear comfortable clothes and sneakers
- Expect about 30–60 minutes total
- You’ll be monitored the entire time
- You can stop if needed
And most importantly:
- You are not alone in that room
- They are watching everything carefully
What I’m Learning Through This
I’m still in the middle of this journey. My next step is my stress echo. But already, a few things feel clear:
- Numbers matter, even when you feel fine
- Early testing is a gift, not a punishment
- You don’t need to panic to take something seriously
And maybe the biggest one: You can be proactive without being fearful